Click here to view this newsletter as a PDF.
Prayer
- For The Lord’s wisdom and guidance in helping to mentor Internal Medicine Residents currently studying in Mbingo Baptist Hospital under CIMS (Christian Internal Medicine Specialization).
- For the responsible use of available supplies and equipment in the midst of the current pandemic – that our staff might be adequately protected.
Praises
- For our very capable Cameroonian colleagues seeking to provide a responsible and measured response to the COVID-19 threat.
- For the innovative efforts of our missionaries who are finding ways to preserve surgical masks such that they can safely be reused.
- For the sovereignty of God, “in whom there is no shadow of turning,” in this changing and turbulent world.
“Jesus Christ is the same yesterday and today and forever.”
hebrews 13:8
 As mentioned in a previous newsletter, I’ve now relocated to Mbingo Baptist Hospital for the purpose of helping with the Internal Medicine Residency being conducted here. On March 12, responsibility for the program was formally handed to me. Pictured above at that time are Dr. Dennis Palmer, current dean of the Baptist Institute of Health Sciences and the former Program Director of CIMS. Dr. Palmer is flanked by Dr. Alfred Njamnshi – a neurologist and former vice dean of the School of Biomedical Sciences in the capital of Yaounde. Dr. Njamnshi is seen addressing the residents.
As mentioned in a previous newsletter, I’ve now relocated to Mbingo Baptist Hospital for the purpose of helping with the Internal Medicine Residency being conducted here. On March 12, responsibility for the program was formally handed to me. Pictured above at that time are Dr. Dennis Palmer, current dean of the Baptist Institute of Health Sciences and the former Program Director of CIMS. Dr. Palmer is flanked by Dr. Alfred Njamnshi – a neurologist and former vice dean of the School of Biomedical Sciences in the capital of Yaounde. Dr. Njamnshi is seen addressing the residents.
Of course, much has happened since then with the advent of COVID-19 disease on the global scene. It was around the time of this handing-over that the first case of COVID-19 was identified in Cameroon. Shortly after this time, in late March, Cameroon closed its borders to international travel. As of May 2, over 2,000 individuals with the coronavirus have been identified in Cameroon.
Our Cameroonian administration was proactive in terms of making preparations to receive patients. Beginning in April, weekly meetings have been held to assess preparedness, establish guidelines for receiving patients, and review stock levels of Personal Protective Equipment (PPE).
 Dr. Nancy Palmer and another innovative missionary started to sew double-layer masks using local African cloth. These were fashioned with a posterior pocket – allowing the standard surgical mask to be inserted inside. This preserved the hospital’s supply of surgical masks – the stock of which was rapidly dwindling as all hospital staff are required to wear masks.
Dr. Nancy Palmer and another innovative missionary started to sew double-layer masks using local African cloth. These were fashioned with a posterior pocket – allowing the standard surgical mask to be inserted inside. This preserved the hospital’s supply of surgical masks – the stock of which was rapidly dwindling as all hospital staff are required to wear masks.
An isolation area was designated and several patients with suspicious symptoms requiring hospitalization have been cared for in that setting. Isolation ward staff wear the more standard PPE, which the hospital is seeking to maintain in stock. Much of our initial stock of PPE remained from 2015 following the Ebola crisis.
Testing for the virus remains a challenge as only one lab in the country initially had this capability. With time, testing has become more widely available. To date, we have not yet identified any Mbingo patients with coronavirus.
Wearing masks throughout the day is our ‘new-norm.’ Often, we need to remind staff to don the face-mask – as these items can feel hot in the midst of work. Our team in Children’s Ward is shown below with one small patient. Gladys is a three-year-old who was admitted in April with a six-month history of generalized seizures. Her mother reported that Gladys often had more than 10 seizures a day. The family initially took Gladys to a witch doctor – who offered various concoctions and assorted remedies to no avail. With time, as a result of the repeated insult to her brain, she became aphasic and profoundly weak. At the time of admission, Gladys was no longer able to talk, walk, or even sit without support.
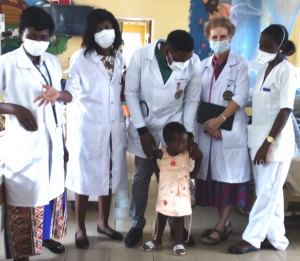 Evaluation revealed no secondary cause of seizure. This little girl appeared to have idiopathic epilepsy. Anticonvulsant therapy resulted in rapid control of her seizures – after which we could only wait, unsure of how much brain damage she had sustained. The team prayed for the child and Glady’s mother was educated regarding her child’s disease. Within five days, Gladys started to recover neurologic function. By the time of discharge she was walking, talking, and playing. We were immensely thankful to God for this outcome.
Evaluation revealed no secondary cause of seizure. This little girl appeared to have idiopathic epilepsy. Anticonvulsant therapy resulted in rapid control of her seizures – after which we could only wait, unsure of how much brain damage she had sustained. The team prayed for the child and Glady’s mother was educated regarding her child’s disease. Within five days, Gladys started to recover neurologic function. By the time of discharge she was walking, talking, and playing. We were immensely thankful to God for this outcome.
Julie Stone
